Why Do My Feet Hurt? Common Foot Pain Causes & Treatment in Mumbai
Most people have asked themselves this question at some point — usually after a long day on their feet, or the moment they take their first steps out of bed in the morning and feel that familiar stab of pain in the heel. Foot pain is one of the most common complaints seen at podiatry clinics in Mumbai, and one of the most consistently ignored.
The problem with ignoring it is straightforward. Your feet take 8,000 to 10,000 steps every single day. Every step you take on a painful, misaligned, or structurally stressed foot is reinforcing the problem — not giving it a chance to resolve. And because your feet are the foundation your entire body moves on, pain that starts in the foot rarely stays there. It works its way upward into the ankles, knees, hips, and lower back over time.
Understanding what is actually causing your foot pain — not just managing the symptom — is the difference between temporary relief and lasting recovery. At Foot Impact, our podiatrists in Mumbai approach every case of foot pain by identifying the root cause first, then building a treatment plan around it. This guide explains the most common causes of foot pain, what each one actually feels like, and how a proper podiatric diagnosis changes the treatment outcome.
Why the Same Foot Pain Keeps Coming Back
Before diving into specific conditions, it's worth addressing the most frustrating experience many patients describe when they first come to Foot Impact — the pain that keeps returning.
Rest makes it better. Activity makes it worse. You try painkillers, a different pair of shoes, maybe some physio. It improves for a few weeks, then comes right back.
The reason this cycle happens is almost always the same: the treatment addressed the symptom but not the cause. Inflammation was reduced, but the mechanical reason the inflammation keeps occurring — a misaligned foot, an overloading gait pattern, a structural issue that puts the wrong kind of stress on the wrong structures with every step — was never identified or corrected.
This is where a computerised gait and pressure analysis makes a fundamental difference. By mapping exactly how your foot is loading during walking — which areas are bearing excessive force, how your arch is behaving, whether you are overpronating or supinating — it becomes possible to identify the specific mechanical driver behind your pain and correct it at the source. Without this data, most foot pain treatment is educated guesswork.
Foot Pain by Location — Find Your Symptom
The most practical starting point for understanding foot pain is where it hurts. Here is a quick guide to the most likely causes based on pain location:
| Where It Hurts | Most Likely Cause | Key Feature |
|---|---|---|
| Under the heel | Plantar fasciitis, heel spur | Worst with first steps in morning |
| Back of the heel | Achilles tendinopathy | Stiffness after rest, worsens with exercise |
| Arch of the foot | Flat feet, plantar fasciitis | Aching after standing or walking |
| Ball of the foot | Metatarsalgia, Morton's neuroma | Burning or sharp pain under the toes |
| Big toe joint | Bunion, hallux rigidus, gout | Visible bump, stiffness, or sudden severe pain |
| Top of the foot | Stress fracture, extensor tendinitis | Pain with specific movements or after running |
| Entire foot / burning | Diabetic neuropathy, nerve entrapment | Tingling, numbness, burning sensation |
| Outer edge of foot | Cuboid syndrome, peroneal tendinitis | Pain after rolling ankle or prolonged walking |
Use this table as a starting point — not a diagnosis. Many conditions overlap in their presentation, and several causes can co-exist in the same foot. What matters is a proper clinical assessment to confirm which structures are involved and why.
The Most Common Causes of Foot Pain — Explained Properly
1. Plantar Fasciitis — The Leading Cause of Heel Pain in India
If your heel hurts most sharply when you take your first steps in the morning, and eases slightly after a few minutes of walking only to return after prolonged activity, plantar fasciitis is the most likely explanation.
The plantar fascia is a thick band of connective tissue running along the sole of your foot from the heel bone to the base of the toes. It supports the arch and absorbs impact with every step. When this tissue is chronically overloaded — through flat feet, overpronation, prolonged standing, or a sudden increase in activity — it becomes inflamed and develops micro-tears that cause the characteristic pain.
What makes plantar fasciitis so persistent is that the plantar fascia never truly gets a chance to rest. Every step reloads it. Without correcting the biomechanical reason it is overloaded — most commonly overpronation or a collapsing arch — it keeps re-inflaming regardless of how much you rest or stretch.
Custom orthotics that control arch loading during every step are the cornerstone of proper plantar fasciitis treatment. Stretching and footwear modification support the recovery, but without addressing the loading mechanics, most cases keep recurring.
Who gets it in Mumbai: Teachers, retail and hospitality workers, healthcare staff, and anyone spending 6–8 hours per day on hard floors — particularly those wearing flat, unsupportive chappals or casual footwear.
2. Flat Feet and Overpronation — The Root Cause Behind Many Conditions
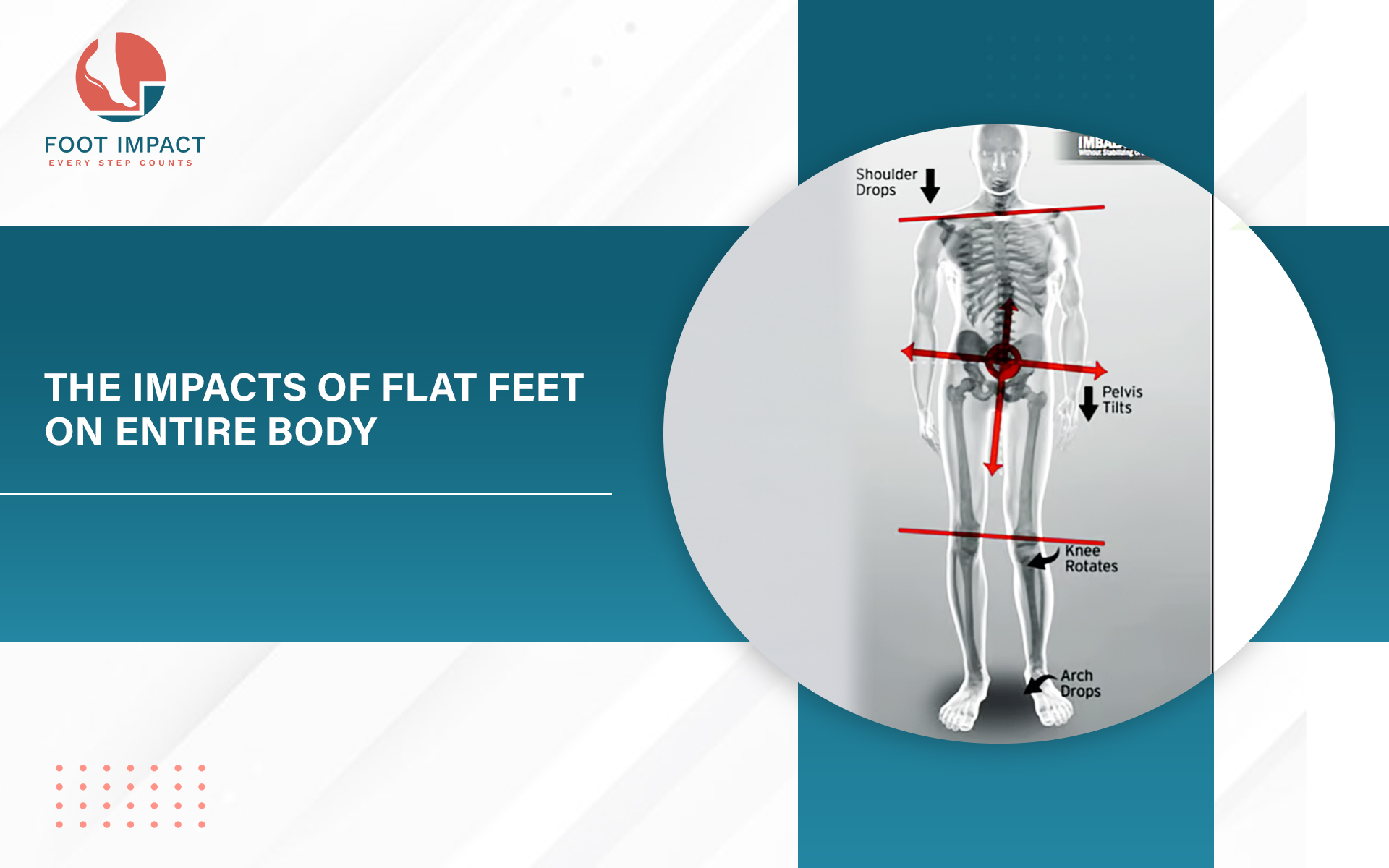
Flat feet — where the arch collapses inward when you stand or walk — is not just a condition in itself. It is one of the most common underlying drivers of multiple foot and ankle problems, including plantar fasciitis, bunions, Achilles tendinopathy, shin splints, and knee pain.
When the arch collapses, the entire foot rolls inward with every step — a pattern called overpronation. This rolling motion creates rotational stress through the ankle, knee, and hip that compounds over thousands of steps per day. The foot and lower limb structures were not designed to sustain this rotational loading continuously, and over time they respond with inflammation, pain, and structural change.
The important distinction is between structural flat feet — where the arch is permanently low — and functional overpronation, where the arch collapses dynamically during walking even if it appears normal when sitting. Computerised pressure mapping identifies both patterns and determines which requires orthotic correction, which requires footwear change, and which requires targeted strengthening.
Key signs you may have flat feet or overpronation: Shoes that wear down disproportionately on the inner heel, ankle pain on the inside, arch aching at the end of the day, and knee pain that worsens with prolonged walking.
3. Metatarsalgia — Pain in the Ball of the Foot
Metatarsalgia refers to pain, burning, or aching in the ball of the foot — the padded area just behind the toes. It is particularly common in people who stand for long periods, wear high heels regularly, or have a foot structure that concentrates excessive pressure on the forefoot.
The five metatarsal bones run from the mid-foot to the toes. When one or more of these bones bears disproportionate load — because of high arches, a dropped metatarsal head, weak forefoot muscles, or footwear that shifts weight forward — the soft tissues beneath them become inflamed and painful.
Metatarsalgia is one of the conditions most commonly mismanaged with cushioned insoles alone. While cushioning reduces impact, it does not correct the underlying load distribution that is concentrating pressure on specific metatarsal heads. A pressure mapping assessment identifies exactly which metatarsals are overloaded and allows an orthotic to be designed that redistributes that load correctly across the forefoot.
Symptom to watch for: Pain or a feeling of walking on a pebble under the ball of the foot, typically worst at the end of the day or after prolonged standing.
4. Achilles Tendinopathy — Not Just an Athlete's Problem
The Achilles tendon — the largest and strongest tendon in the body — connects the calf muscles to the heel bone and passes directly behind the ankle. Pain, stiffness, or swelling in this area, particularly in the morning or after periods of rest, is the hallmark of Achilles tendinopathy.
Despite its reputation as a runner's injury, Achilles tendinopathy is increasingly common in non-athletes — particularly adults who have recently increased their activity levels, returned to exercise after a long break, or spend long hours in flat footwear that provides no calf-Achilles support. Overpronation also contributes directly, as the inward rolling of the foot during walking places asymmetric rotational stress on the Achilles at every step.
The most important thing to understand about Achilles tendinopathy is that it does not respond to rest in isolation. The tendon fibres need graduated loading to heal properly — the right kind and amount of movement, not simply stopping activity. A podiatrist-guided rehabilitation programme, often combined with heel raise devices or orthotics to reduce Achilles load during recovery, produces reliably better outcomes than rest and hope.
Warning sign: A complete Achilles tendon rupture — a serious injury requiring surgical intervention — is significantly more likely in tendons that have been chronically inflamed and inadequately treated. If your Achilles has been painful for months, get it properly assessed.
5. Diabetic Neuropathy and Diabetic Foot Pain
India has one of the highest rates of diabetes in the world — and diabetic foot complications are one of the most serious and preventable consequences of poorly managed diabetes.
Diabetic neuropathy causes nerve damage in the feet, producing burning, tingling, numbness, or shooting pain — often described as an electric sensation or the feeling of walking on sand. What makes diabetic foot pain particularly dangerous is the other side of neuropathy — reduced sensation. When the nerves that carry pain signals are damaged, cuts, blisters, pressure sores, and ulcers can develop and worsen without the patient feeling them.
A pressure sore that a person without diabetes would notice and address immediately can, in a diabetic patient, progress to a deep wound and serious infection before it is detected. This is the pathway that leads to the amputations that represent the most severe end of diabetic foot complications.
Regular podiatric check-ups for all diabetic patients are not optional — they are essential preventive care. At Foot Impact, diabetic foot assessments include pressure mapping, sensation testing, vascular assessment, and footwear review as standard.
If you have diabetes and notice any change in your feet — no matter how minor it seems — seek assessment within days, not weeks.
6. Bunions — Progressive Joint Misalignment
A bunion (hallux valgus) is a structural misalignment of the big toe joint, visible as a bony bump on the inner side of the foot. It develops gradually as the first metatarsal bone drifts inward while the big toe angles toward the second toe — a process driven primarily by foot biomechanics and genetic predisposition, accelerated by narrow or high-heeled footwear.
Bunions do not resolve on their own. The forces of walking act continuously on the joint, and without intervention to correct the underlying mechanics, the misalignment progresses steadily. The majority of bunion cases — including many moderate ones — can be effectively managed without surgery through custom orthotics, footwear correction, and targeted exercise.
For a complete explanation of bunion causes, staging, and treatment options, see our dedicated guide: Bunion Treatment in Mumbai — Causes, Symptoms & Non-Surgical Options.
7. Arthritis of the Foot and Ankle
Arthritis in the foot presents as deep, aching joint pain that is typically worst in the morning, eases with gentle movement, but worsens again after prolonged activity. Swelling, reduced range of motion, and a gradual increase in stiffness over months or years are characteristic features.
Osteoarthritis — the wear-and-tear type — commonly affects the big toe joint and ankle, particularly in people with a history of foot injuries, chronic biomechanical overloading, or previous joint damage. Rheumatoid arthritis — an autoimmune condition — frequently affects multiple joints in the feet symmetrically and may be accompanied by systemic symptoms like fatigue and morning stiffness in other joints.
Conservative podiatric management through custom orthotics, footwear modification, and activity adjustment can significantly reduce the daily impact of foot arthritis and slow its progression. The sooner loading patterns are optimised, the slower joint deterioration tends to be.
8. Corns, Calluses, and Skin-Related Foot Pain
Corns and calluses are the foot's defensive response to chronic friction and pressure. They are not random — they form precisely where mechanical stress is concentrated, making them useful diagnostic indicators of underlying loading problems.
A corn or callus under the ball of the foot points to metatarsal overloading. One on the inner heel suggests pronation stress. Between the toes, they indicate toe compression — often from narrow footwear. Treating the skin lesion without addressing its mechanical cause means it returns reliably within weeks.
At Foot Impact, corns and calluses are treated as symptoms, not primary problems — the pressure mapping that identifies their cause is as important as the treatment itself.
9. Vitamin D and B12 Deficiency — The Overlooked Systemic Cause
This is one of the most under-recognised causes of generalised foot pain and fatigue in India. Vitamin D deficiency is extremely prevalent in urban Indian adults — counterintuitively, despite high sun exposure, because most urban professionals spend the majority of daylight hours indoors.
Vitamin D deficiency causes diffuse musculoskeletal pain, bone tenderness, and fatigue that is frequently felt in the feet — particularly in the heels and arches. It is commonly misdiagnosed as plantar fasciitis because the symptom pattern overlaps. Vitamin B12 deficiency causes peripheral neuropathy — the same tingling, burning, and numbness in the feet associated with diabetic nerve damage — and is particularly common in vegetarians and the elderly.
If your foot pain is generalised, affects both feet equally, is associated with fatigue or bone tenderness, and has not responded to local treatment, a simple blood test for Vitamin D and B12 levels is worthwhile before pursuing more complex interventions.
How Foot Impact Diagnoses and Treats Foot Pain in Mumbai
The most important thing that separates effective foot pain treatment from ineffective treatment is the starting point — accurate diagnosis.
At Foot Impact's clinics in Andheri West and Khar West, Mumbai, every new patient presenting with foot pain goes through:
Clinical History: How long the pain has been present, what makes it worse and better, occupational demands, activity levels, footwear habits, and any relevant medical history including diabetes, arthritis, or previous injuries.
Physical Examination: Assessment of foot structure, arch type, joint range of motion, tenderness mapping, skin and nail assessment, and basic neurological and vascular screening where indicated.
Computerised Gait and Pressure Analysis: Real-time foot pressure mapping and motion analysis identifies exactly how your foot is loading — which structures are being overloaded, whether overpronation or supination is present, and whether asymmetries in load distribution are driving your symptoms. This is the data that makes the treatment specific rather than generic.
Footwear Assessment: Your current footwear is reviewed. The wrong shoes can undo the benefits of even correctly prescribed orthotics — and for many patients, footwear change alone produces significant improvement.
Personalised Treatment Plan: Based on the full assessment, a specific treatment plan is built around your condition, foot type, lifestyle, and goals — not a standard protocol applied to everyone with the same complaint.
👉 Book Your Foot Pain Assessment at Foot Impact, Mumbai →
When to Stop Managing Foot Pain Yourself and See a Podiatrist
Self-management — rest, ice, over-the-counter pain relief, changing shoes — is reasonable for very recent, clearly minor foot pain. It is not appropriate for:
- Pain that has been present for more than 2–3 weeks without meaningful improvement
- Pain that keeps returning after periods of rest
- Any foot pain in a person with diabetes — regardless of severity
- Swelling, redness, or warmth in a joint that appeared without obvious trauma
- Pain that is affecting your sleep, work, or daily movement
- Any wound or ulcer on the foot that is not healing normally
- Foot pain in a child that is persistent or causing a change in walking pattern
The consistent finding at Foot Impact is that patients who present early — when the problem is new and the mechanics are not yet significantly reinforced — respond faster, require less intervention, and have better long-term outcomes than those who have been managing independently for months or years.
Frequently Asked Questions About Foot Pain
Q1. Why does my foot hurt only in the morning and then ease off? This is the classic pattern of plantar fasciitis. During sleep, the plantar fascia contracts slightly in a shortened position. The first steps of the morning stretch it abruptly, causing pain. As you walk, it gradually warms and loosens — which is why the pain often eases after 10–15 minutes. The easing of pain does not mean the problem has resolved. The tissue remains inflamed and overloaded, and the pain typically returns after prolonged activity.
Q2. Can foot pain cause knee or back pain? Yes — and this is one of the most commonly overlooked connections in musculoskeletal health. When the foot overpronates or the arch collapses, the inward rolling motion is transmitted up the kinetic chain — rotating the shin, loading the inner knee, and affecting hip and lower back alignment. Patients with chronic knee pain or lower back pain that has not responded to local treatment are frequently found to have unaddressed foot biomechanics as a contributing factor.
Q3. Is it better to see a podiatrist or an orthopaedic doctor for foot pain? For the vast majority of foot pain presentations — plantar fasciitis, flat feet, bunions, metatarsalgia, Achilles tendinopathy, and neuropathy — a podiatrist is the right first step. Podiatrists specialise exclusively in foot and lower limb biomechanics and take a non-surgical, root-cause approach. Orthopaedic surgeons are the appropriate referral when imaging confirms a structural problem requiring surgical intervention — which represents a minority of foot pain cases. See our detailed comparison: Orthopaedic Foot Surgeon vs Podiatrist — Who to Visit First.
Q4. Why does my foot pain keep coming back after treatment? Almost always because the underlying mechanical cause was not identified or corrected. Pain medication reduces inflammation. Rest reduces load temporarily. Stretching improves tissue flexibility. But none of these interventions correct a collapsing arch, an overpronating gait, or a structural misalignment that is re-creating the same stress on the same tissues with every step. Computerised pressure mapping is the tool that identifies exactly what is driving the recurrence — and custom orthotics prescribed from that data are what corrects it.
Q5. Can children get foot pain from flat feet? Yes — and childhood is actually the best time to address flat feet and associated pain, because the foot is still developing and orthotic intervention during growth produces better long-term structural outcomes than intervention in adulthood. Children who complain of foot or leg pain after activity, refuse to walk long distances, or walk with an intoeing or outtoeing pattern should be assessed by a podiatrist. Growing pains are real, but persistent, location-specific pain in a child's foot is not simply something to wait out.
Q6. How long does foot pain treatment take to produce results? For biomechanically driven conditions — plantar fasciitis, flat feet, metatarsalgia — most patients notice meaningful improvement within 4–6 weeks of wearing correctly prescribed custom orthotics and modifying footwear. More complex conditions like Achilles tendinopathy typically take 8–12 weeks of graduated rehabilitation. Diabetic foot management and arthritis are ongoing — the goal is symptom control, functional improvement, and slowing progression, not a defined endpoint. What consistently shortens recovery time is starting the right treatment early rather than waiting.
Conclusion — Foot Pain Has a Cause, and the Cause Has a Solution
There is no such thing as foot pain that simply appears for no reason. Every ache, every sharp stab in the heel, every burning sensation in the toes has a structural or biomechanical explanation — and that explanation is findable with the right assessment.
What the patients who come to Foot Impact in Mumbai consistently tell us is not just that the pain improved — it's that for the first time, someone explained why it was happening. That understanding, combined with a treatment plan built around the actual cause, is what turns chronic recurring foot pain into a resolved problem.
If your feet have been telling you something is wrong — whether for weeks, months, or years — now is the right time to listen properly.
Book your foot pain assessment at Foot Impact, Andheri West, Mumbai →